It’s common knowledge that birth control prevents pregnancy, but have you ever considered how your contraceptive actually works with your body? Read on to find out more about the ins and outs of contraceptives.
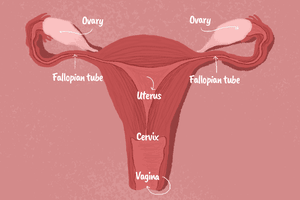
A pregnancy occurs as a result of a three-step process – ovulation, fertilization, and implantation. Hormones cause the ovaries to release a mature egg (ovulation), which then joins with a sperm cell (fertilization), and implants itself into the lining of the uterus (implantation). Once implanted, the egg begins growing into a fetus and the pregnancy begins.
To prevent a pregnancy from occuring, contraceptives stop the process of fertilization; but the actual mechanism varies from one contraceptive to another. Broadly speaking, there are five different mechanisms for inhibiting fertilisation: preventing ovulation, incapacitating sperm, thickening the cervical mucus, blocking the sperm, and sterilization. It’s important to note that most contraceptives use more than one of these mechanisms.
Here is a closer look into how these mechanisms work:
1. Preventing ovulation
The normal menstrual cycle has different phases, which begin and end based on changes in hormone levels. Modifying these regular functions of the body prevents ovulation.
Usually, a rise in hormone levels sends a message to the pituitary gland, which in turn sends a signal to the ovaries to release an egg. In order to stop this from happening, synthetic forms of the hormones progesterone and estrogen are used to suppress the rise of hormone levels in the body. Without the usual cyclical surge in hormones, ovulation does not occur. If no egg is released for the sperm to fertilize, a pregnancy cannot occur.

Contraceptive methods that prevent ovulation include the combined pill, progestin-only pill (also known as mini pill), emergency contraceptive pill, ring, implant, injection, and the Lactation Amenorrhea Method (LAM) – a temporary method for breastfeeding mothers founded on the natural infertility that arises while breastfeeding and when menstrual bleeding has stopped (amenorrhea).
2. Incapacitating sperm
Disabling the sperm before it can fertilize the egg is another way of preventing pregnancy. Spermicides create such a chemical barrier between the sperm and the egg.
Spermicide comprises chemicals, such as nonoxynol-9, that contain surfactants that cause the membranes of the sperm cells to rupture. This slows the sperm down and stops it from entering the uterus. When used correctly, spermicide blocks the cervix so that sperm can’t reach the fallopian tubes or uterus. It also alters the pH of the vagina, which creates an unfavourable environment for the sperm.
Spermicide is often used together with a mechanical barrier method to prevent pregnancy, such as a cervical cap, condom, or diaphragm. It comes in many different forms, including as a foam, film, gel, cream, or suppository.

3. Thickening of the cervical mucus
The cervix discharges a fluid called the cervical mucus. The consistency, color, and volume of cervical mucus changes throughout the month, depending on your hormones and where you are in your menstrual cycle. The main purpose of the mucus is to help transport the sperm to the egg. During ovulation, the cervical mucus is usually slippery and stretchy. This is the ideal consistency to deliver the sperm to the egg.
Contraceptives that thicken the cervical mucus obstruct this process. They cause the cervical mucus to become much thicker, which makes it more difficult for sperm to penetrate the uterus, and reach and fertilize the egg, and for the egg to attach to the lining of the uterus.

There are several contraceptives that thicken the cervical mucus to prevent fertilisation. They include the pill, mini pill, implant, and the copper and hormonal intrauterine device (IUD).
4. Blocking sperm
Barrier methods of contraception block sperm from passing through the cervix into the uterus. Mechanical barriers block sperm from reaching and fertilizing the egg by providing a physical barrier between the two. If the sperm can’t reach the egg, then a pregnancy cannot occur.

Contraceptive methods that block sperm are the male and female condom, as well as the diaphragm, sponge, and cervical cap. Latex, thin plastic (polyurethane), soft silicone, or synthetic rubber (polyisoprene) are the most common materials for these methods. These impenetrable materials prevent contact between the sperm and the vagina. Sometimes, they are covered with spermicide too.
5. Sterilization
The most effective way to prevent fertilization is via sterilization, which is a permanent method of birth control. For women, this can be done via a hysterectomy or through “tying the tubes” (tubal ligation). For men, sterilization is done through a vasectomy.
There are different types of hysterectomies – for example, partial or total hysterectomy. In a total hysterectomy, the surgeon removes the uterus, including the cervix and possibly the ovaries and fallopian tubes. After this, the menstrual cycle will cease and a pregnancy will not be able to occur. In a partial hysterectomy, the doctor only removes the upper cervix.

Tubal ligation is a surgical procedure in which the surgeon cuts, cauterizes, or bands the fallopian tubes. As a result, eggs can’t travel to the uterus and get fertilized.
In a vasectomy, the doctor cuts and then ties or sears the tubes (vasa deferentia) that transport sperm from the testes. After a vasectomy, the testes still produce sperm but the sperm dies and the body reabsorbs it before it can fertilize an egg.

There are so many contraceptives available that it can be overwhelming to come to grips with the mechanics of each one. However, knowing more about how each method functions, as well as how each contraceptive affects your body, can make all the difference when it comes to choosing a contraceptive that is right for you and your lifestyle.
Do you have something to share? Leave your comments below, contact us on our social media platforms: Facebook, Instagram and Twitter or send us an email to info@findmymethod.org. For more information on contraception, visit findmymethod.org
About the author: Julia Riccardi is a freelance writer and editor based in Johannesburg, South Africa. She has a BA in English and Comparative Religion and a passion for words, people, and holistic health.